 Despite all the glamorous marketing campaigns and advertising creatives that promote alcohol as a casual comfort of life, people should know that even just a small bit could bring about a number of adverse conditions, not the least of which are skin conditions from alcoholism.
Despite all the glamorous marketing campaigns and advertising creatives that promote alcohol as a casual comfort of life, people should know that even just a small bit could bring about a number of adverse conditions, not the least of which are skin conditions from alcoholism.
Even worse is the fact that for other people, the adverse conditions brought about by alcohol could either be progressive in nature and get worse over time, or cause permanent damage that no amount of treatment could fix.
This is why people should really put more thought into how much alcohol they take since the popular advice of “drinking moderately” could be entirely subjective to how a person’s body reacts to the alcohol. If you or someone you love is dealing with alcoholism, please contact us today to find out more about our Illinois alcohol rehab center.
What Skin Conditions Does Alcohol Bring?
Truth be told, there are a number of skin conditions that are generally associated with the chronic intake of alcohol, although dermatologists and medical professionals have their own opinion as to which ones could really be attributed solely to alcohol and not to other reasons.
The most basic adverse effect of alcohol on the body is dehydration. This is because of two reasons, both of which actually compound each other. Alcohol in itself is a potent diuretic and is believed to be many times more powerful as a diuretic than coffee. As such, drinking alcohol causes the body to expel more fluids than normal through frequent urination.
The second reason for dehydration has to do with the toxic effect of alcohol on the body. The human body will normally flush out any toxic substance that starts to do harm to it. As alcohol is toxic, the body will naturally do its best to flush out as much of it as it can.
These two factors typically combine when a person drinks alcohol and ensures that dehydration is soon to follow. This is why people who have had too much to drink experience a hangover. The ill feeling is from the body being deprived of too much liquid. Dehydration affects the entire body, including the skin, causing it to lose its natural elasticity and resilience, making it look dull and dry.
As the skin loses moisture due to dehydration, the cells that make up the skin begin to age and die prematurely. Skin cells have a normal cycle of drying out and sloughing off once the new skin cells underneath it are ready to become the surface layer.
When the skin becomes excessively dry due to dehydration, the surface layer dies off and becomes dull, weathered, and flaky. If it does not slough off immediately, it forms a rough, leathery epidermis that looks more suited to a dead body than it does to a living person.
In other instances, the dead skin sloughs off sooner than it should, revealing the layer beneath that is not yet ready and acclimated to become the surface layer, resulting in highly sensitive and tender skin that could easily be cut or broken by simple abrasion.
In instances where the skin does not peel off once the surface layer is dead, it forms a leathery surface that could either be darker than the normal hue of healthy skin or be unevenly discolored.
Despite the fact that this type of dry skin feels leathery, it is not as durable as traditional leather. It could still be cut or flaked off in sections where the skin surface has already been broken. This condition could typically be addressed with skin moisturizers, but if the person continues with chronic alcohol intake, there could be no marked improvement in skin quality.
Apart from the obvious reason for bruised skin for heavy drinkers, which is usually because of frequent falls or blunt trauma from bumping into things while drunk, bruising is also a common skin condition for most drinkers.
This is attributed to scurvy brought on by a deficiency in vitamin C. Alcoholism is largely blamed for a number of vitamin deficiencies, with the most dangerous being Thiamine deficiency.
As alcohol intake also depletes the body of vitamin C, bruising becomes quite common, which is alarming as it could mask other conditions that also result in bruises on the body.
Alcohol is also known to severely compromise the immune function of the body, increasing a person’s susceptibility to infections. Alcohol compromises the immune system in two ways: it could directly impair the immune system due to its toxicity, and it could also bring about impairment due to vitamin deficiency, particularly vitamin C and zinc, both of which are needed to maintain a strong immune system.
As skin integrity is also compromised from the effects of alcohol, it becomes highly susceptible to cuts and breaks, which gives bacteria an easy way in. Depending on how compromised the immune system is, a person could suffer a serious infection this way.
Heavy drinking is known to increase the chances of a person developing cancer, particularly the ones that affect the mouth and the digestive system. In an indirect way, however, chronic drinking also puts a person in danger of developing skin cancer as well.
As skin becomes increasingly damaged through dehydration, it also becomes increasingly susceptible to DNA damage caused by excessive exposure to ultraviolet rays. This is particularly true with cases of both malignant melanoma and non-melanoma skin cancers, as there is research suggesting that chronic alcohol intake significantly increases the chances of developing either form of skin cancer.
Another added factor is that chronic drinkers also tend to be greater risk takers, including the risk of extended exposure to the sun despite having severely dehydrated skin. This extended exposure further increases the chances of developing skin cancer as the person cares less about being careful and care more about getting inebriated.
Over time, alcohol damages most of the major organs in the body. One of the very first organs to suffer the most damage is the liver, and increased liver damage tends to affect the body in numerous ways, including manifestations on the skin.
Jaundice is the discoloration of the skin, giving a person a noticeably yellowed skin tone. This skin discoloration is an indicator that the liver has already been damaged by the excessive intake of alcohol. In some cases, once the person manifests jaundice, the damage is already at a severe level and could become life-threatening.
Heavy alcohol intake is also known to trigger a psoriasis outbreak, a manifestation of a skin disease that causes numerous rashes characterized by itchy, scaly patches. These patches typically appear on the knees, elbows, trunk, and scalp.
Psoriasis is a common, long-term disease for which there is no known cure. In some cases it could be painful to the point that it interferes with sleep and persist during the waking hours, making it hard to concentrate. To date, there have been no conclusive findings as to what causes it, although researchers are looking at a possible scenario where the body’s infection-fighting cells attack healthy skin cells.
Another danger that comes with dehydrated skin is the increased chance of contracting cellulitis. Cellulitis is a common, potentially serious bacterial skin infection that is caused by bacteria, most commonly streptococcus and staphylococcus, that get into the skin through a crack or break.
As dehydrated skin lacks the natural resilience that healthy, moisturized skin has, it easily breaks from simple abrasion, offering an entry point for bacteria. The affected skin then becomes swollen, inflamed, and painful. If left untreated, the infection could spread to the lymph nodes and bloodstream and even become life-threatening quite quickly.
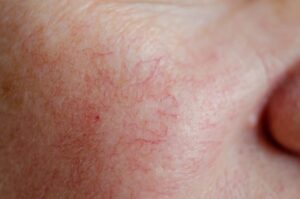
People who have a red, swollen, and bumpy nose were initially thought to be heavy drinkers, which is why this condition has come to be called “alcoholic nose.” This condition is more properly known as rhinophyma, which is an advanced stage of rosacea, another skin condition that causes blushing or flushing and visible blood vessels in the face. In some cases, it also produces small, pus-filled bumps that may stay for up to weeks at a time.
Some people, however, do get a red and stuffy nose when they drink. This is largely associated with being an allergic reaction to alcohol and is most common in people with asthma, sinus diseases, and a great tendency to manifest an allergic reaction to substances like alcohol.
What is the Treatment for Skin Conditions Caused by Alcoholism?
 The very first treatment required to stop the progression of alcohol-driven skin conditions is to stop taking the cause of the condition: alcohol. While there are some people who manage to stop their alcoholic habits on their own, the best way to go about it is through our alcohol and drug detox center in Illinois, with additional support options like sober living in Illinois to provide structure and guidance in overcoming alcohol abuse. It is also designed to manage any medical complications that might arise during the process, and you can take our Drug Addiction Quiz to better understand your risk while seeking help.
The very first treatment required to stop the progression of alcohol-driven skin conditions is to stop taking the cause of the condition: alcohol. While there are some people who manage to stop their alcoholic habits on their own, the best way to go about it is through our alcohol and drug detox center in Illinois, with additional support options like sober living in Illinois to provide structure and guidance in overcoming alcohol abuse. It is also designed to manage any medical complications that might arise during the process, and you can take our Drug Addiction Quiz to better understand your risk while seeking help.
Following the completion of the medical detox is rehabilitation, where the person looking to quit alcohol is given therapy to deal with the urges to take alcohol once more, and also to help build a mindset and attitude that will allow them to cope with life and other stressors without having to resort to alcohol.
Find Help With Northern Illinois Recovery
Alcohol is one of the most difficult substances to quit, and also one of the easiest to get back in. This is why so many people suffer an almost immediate relapse after having completed one form of alcohol rehab or another. This is why we here at Northern Illinois Recovery put greater effort into helping people develop a healthy understanding of the problem and an even greater appreciation of how better life would be if they stick to the path to sobriety.
Some people with an alcohol abuse disorder never get a second chance to fix things, which is why we do our best to get it right the first time around. Talk to us now.





